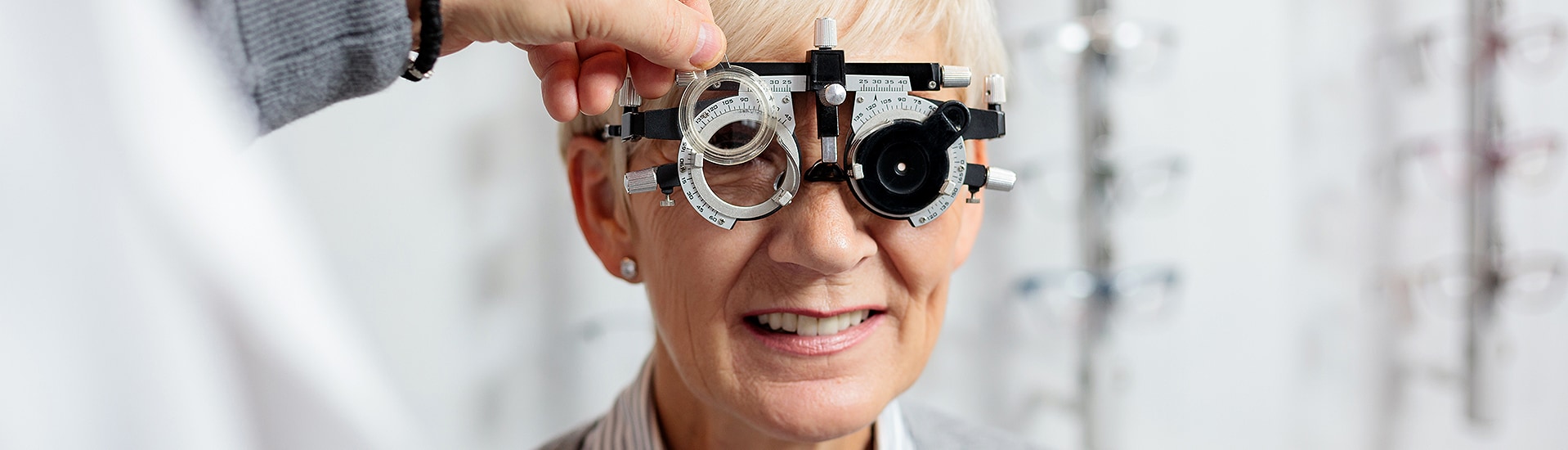
Yearly Diabetic Eye Exams Can Save Your Sight
Diabetic eye examinations can help prevent eye complications related to diabetes type 1 and 2. Diabetes can cause multiple ocular complications, including vision loss. It may also worsen pre-existing vision problems, such as myopia (nearsightedness), hyperopia (farsightedness), and presbyopia.
Regardless of type, all people with diabetes should have yearly eye assessments to protect their eye health.


What Is Diabetic Eye Disease?
Diabetic eye disease is a group of eye problems caused by diabetes. The 4 conditions include:
- Cataracts
- Diabetic macular edema
- Diabetic retinopathy
- Glaucoma
Diabetic eye disease develops over time. Patients may not notice immediate symptoms or changes to vision. However, as blood glucose (blood sugar) levels remain high, it can damage blood vessels in the eye. The damage can affect the normal function of your eyes, interfering with sight and eye health.
Cataracts
Cataracts are cloudy or foggy spots that form in the normally clear lens of your eye. The cloudy spots can vary in size, affecting vision differently depending on how the cataract develops over time. Cataracts can affect anyone, but high blood sugar levels increase the risk.
Cataract symptoms include:
- Blurry or foggy vision
- Poor colour vision
- Decreased night vision
- Halos around lights
- Light sensitivity
- The feeling of a film over the eye
Treatment for cataracts depends on how severely vision is impacted and the patient’s comfort level. Prescription lenses or cataract surgery are 2 common treatment options.
Diabetic Macular Edema
Macular edema or diabetic macular edema (DME) affects the health and function of the macula. The macula, located in the retina, allows us to see central (straight-ahead) vision as well as most of our colour vision. Eye conditions damaging the macula do not affect peripheral (side) vision.
Diabetic macular edema results from excess fluid buildup around the macula. High blood sugar levels cause damage to blood vessels in the back of the eye (diabetic retinopathy), leading to fluid leaking and tissue swelling. The increased fluid buildup causes the macula to swell and thicken.
Symptoms of macular edema include:
- Blurry or wavy central vision
- Washed out or faded colours
Treatment for diabetic macular edema can include laser therapy and injectable medications.
Diabetic Retinopathy
Diabetic retinopathy (DR) occurs when high blood sugar causes damage to blood vessels in the retina. The retina is a crucial part of our visual system, as it receives and converts light into signals for our brain. More than 500,000 Canadians are living with diabetic retinopathy.
Symptoms of diabetic retinopathy include:
- Blurry vision
- Dark spots or holes in vision
- Flashes of light
- Loss of central vision
- Inability to see colours
Diabetic retinopathy also increases the risk of other eye complications, including retinal detachment.
Early detection is crucial in preventing vision loss. In the early stages of the eye disease, symptoms can be managed by controlling blood pressure and blood sugar. As the disease progresses, options to prevent vision loss include:
- Anti-VEGF injections
- Retinal photocoagulation (laser therapy)
Vitrectomy (surgery)
Retinal Detachment
As diabetic retinopathy develops, it damages blood vessels in the back of the eye, the location of the retina. The retina is crucial to functioning vision, however, the tissue is delicate. Fluid leakage can cause the retina to lift away from the back of the eye and detach.
Common symptoms of retinal detachment include:
Some patients describe the decreased vision like a curtain or veil descending over their field of vision.
It’s crucial to seek immediate medical attention after retinal detachment. Surgery can repair 90% of detachment cases. Success can depend on the severity of the tear, scar tissue, and whether the macula was affected. The sooner a patient receives treatment, the better the chances of success.
Contact us for an emergency eye appointment if you experience sudden vision loss, flashes, or floaters.
Glaucoma
Glaucoma is a group of eye diseases. Diabetes is a significant risk factor for developing glaucoma. Increased blood sugar levels damage blood vessels in the eye and lead to abnormal blood vessel growth. The abnormal growth can block fluid from draining, increasing intraocular pressure (IOP).
Higher IOP is the main cause of most types of glaucoma. The pressure can damage the optic nerve, leading to blindness. Early detection is crucial to preventing vision loss.
Treatment options for glaucoma include:
- Drainage implants
- Medications
- Laser surgery
- Trabeculectomy
Diagnosing Diabetic Health
Our eye care team may use various diagnostic methods and technologies to look at your eye health. OCT and digital fundus imaging are 2 technologies we use during a diabetic eye examination.
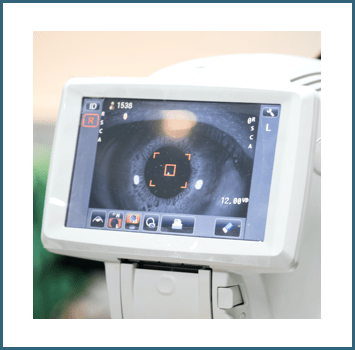
OCT
Optical coherence tomography (OCT) is an imaging test that uses light waves to take cross-section pictures of the retina and optic nerve. It creates high-quality images, allowing for detailed measurements of the retina and eye structures.
An OCT scan is a noninvasive test requiring pupil dilation. The scan typically lasts between 10–15 minutes.
Digital Fundus Imaging
The fundus is the back surface of the eye and it includes the retina, macula, optic nerve, fovea, and blood vessels. Fundus imaging uses a low-power microscope to photograph the interior surface and back of the eye.
Digital fundus imaging is a noninvasive test and can be completed in a few minutes. As the images are taken through the pupil, pupil dilation is necessary to provide the camera with a better opening to look through.
Preventing Diabetic Eye Disease
Yearly diabetic eye examinations are a crucial part of preventing eye disease and other complications of diabetes. Westmount Optometrists can help you protect your vision through diagnosis and treatment. The sooner we see you, the sooner we can work together to protect your eyes.
Book a diabetic eye examination today. Trust us, you’ll see!

Frames We Love!





Where To Find Us
At the corner of Springbank Drive and Wonderland Road, our clinic offers plenty of parking out front.

Our Address
- 585 Springbank Dr.
- London, ON N6J1H3
Talk to Us
- Phone: 519-472-0210
- Email: [email protected]
Our Hours
- Monday: 8:00 AM – 7:30 PM
- Tuesday: 8:00 AM – 7:30 PM
- Wednesday: 8:00 AM – 7:30 PM
- Thursday: 8:00 AM – 7:30 PM
- Friday: 8:00 AM – 5:00 PM
- Saturday: Closed
- Sunday: Closed
Read Our Blog
What Are Myopia Glasses?
Children’s Eye ExamThese eyeglasses use specially designed lenses that cause light to focus on the eye in a way that slows myopia progression in children.
[…]
Dry Eyes or Allergies: How to Identify the Cause of Your Eye Discomfort
Contact Lenses, Digital Eye Strain, Dry Eye, Eye Care, Eye Exams, Eye HealthThe key difference? Dry eyes are typically caused by poor tear production or when your tears evaporate too quickly, while eye allergies result from your immune system reacting to allergens like pollen or dust. The symptoms may overlap, but the causes—and treatments—are very different.
[…]
How Do You Know if Sunglasses Are Polarized?
SunglassesOne of the easiest ways to determine if your sunglasses are polarized is by using the reflection or screen test. […]
What Are Myopia Glasses?
These eyeglasses use specially designed lenses that cause light to focus on the eye in a way that slows myopia progression in children.
[…]
Dry Eyes or Allergies: How to Identify the Cause of Your Eye Discomfort

The key difference? Dry eyes are typically caused by poor tear production or when your tears evaporate too quickly, while eye allergies result from your immune system reacting to allergens like pollen or dust. The symptoms may overlap, but the causes—and treatments—are very different.
[…]
How Do You Know if Sunglasses Are Polarized?

One of the easiest ways to determine if your sunglasses are polarized is by using the reflection or screen test. […]